Introduction
A frequent condition that hurts the heel and sole of the foot is plantar fasciitis. It happens when the thick band of tissue known as the plantar fascia, which connects the heel bone to the toes, is swollen or injured. Numerous things, such as overuse, high-impact activities, flat feet, and tight calf muscles, might be the result of this.
Plantar fasciitis can develop chronic and interfere with everyday activities if it is not treated. However, there are certain methods by which plantar fasciitis can be treated in a week. People suffering from plantar fasciitis might find relief from their pain and discomfort by knowing the disease and taking the appropriate action.
Before we dive into the comprehensive guide, it’s vital to remember that foot pain is an intense sensation, as your entire body weight rests upon your feet. I implore you to avoid uncomfortable shoes, especially trekking or high-heeled shoes, as these can exacerbate your condition, particularly when navigating stairs where a sudden twist can strike at any moment.
In this article, I will be discussing Plantar Fasciitis, its types, causes and symptoms, diagnosis for plantar fasciitis, stages of plantar fasciitis, treatment methods for plantar fasciitis, alternative treatment methods, short-term vs long-term relief from plantar fasciitis, preventions to be taken, nutrition to be taken for plantar fasciitis, potential risks and case study related to plantar fasciitis.
I will also be discussing How to Cure Plantar Fasciitis in One Week – a one-week Treatment Plan. Is it possible to Cure Plantar Fasciitis in One Week? If yes, how?
In this detailed guide, I am thrilled to share my personal journey and the steps that helped me bid farewell to Plantar Fasciitis in just one week. If you’re eager to learn how I regained my stride and bid adieu to foot pain, continue reading. Your path to relief and recovery may be shorter than you ever imagined.”
Do Read the People Also Ask (FAQs) about this topic.
Key Takeaways
- A frequent condition that hurts the heel and sole of the foot is plantar fasciitis.
- People suffering from plantar fasciitis might find relief from their pain and discomfort by knowing what is causing it and taking the appropriate action.
- People can stop plantar fasciitis from recurring or developing by receiving the appropriate care and taking preventative measures.
Understanding Plantar Fasciitis
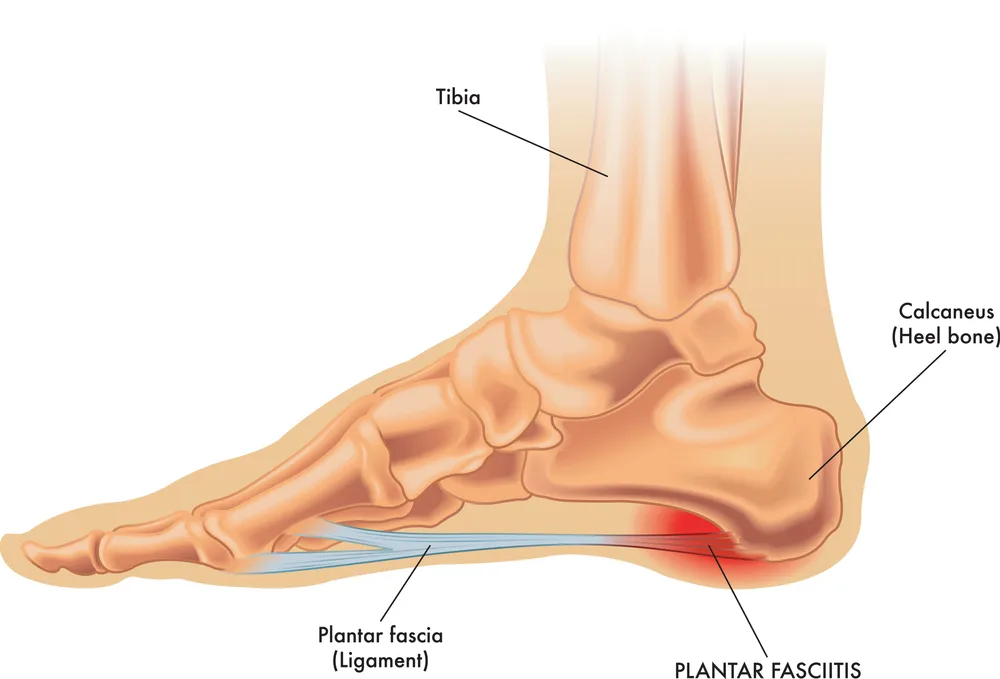
What is Plantar Fasciitis?
Plantar fascia, a thick band of tissue that spans the bottom of each foot, is a frequent foot disease called plantar fasciitis. The plantar fascia supports the foot arch and links the heel bone to the toes. The plantar fascia can become inflamed and hurt the heel or arch of the foot if it is stressed.
Regardless of age or degree of activity, anyone can get plantar fasciitis. It is particularly prevalent in runners, overweight individuals, and wearers of inadequately supportive footwear. The discomfort may be modest to severe, and the disease may be transient or persistent.
Pain in the heel or arch of the foot, especially when standing or walking, is one of the signs of plantar fasciitis. After spending a lot of time sitting or standing, the discomfort could be severe in the morning. In rare circumstances, the discomfort in the affected area could also be accompanied by swelling or redness.
Types of Plantar Fasciitis
A frequent condition that affects the foot is plantar fasciitis. The plantar fascia, a substantial band of tissue that runs along the bottom of the foot, becomes inflamed, giving rise to the condition. Numerous causes, such as excessive use, improper foot mechanics, and specific medical conditions can contribute to plantar fasciitis. There are two types of plantar fasciitis: acute and chronic.
- Acute Plantar Fasciitis
- Chronic Plantar Fasciitis
1. Acute Plantar Fasciitis
Foot pain that develops suddenly is known as acute plantar fasciitis. It typically occurs by a particular incident, like an abrupt surge in activity or a traumatic accident. With rest and the right care, acute plantar fasciitis typically goes away on its own within a few weeks.
2. Chronic Plantar Fasciitis
Chronic plantar fasciitis is a long-lasting ailment that causes constant foot pain. Overuse or repetitive stress on the foot are the usual causes. It can be challenging to treat chronic plantar fasciitis, which may call for more drastic measures like physical therapy or surgery.
It’s vital to remember that plantar fasciitis can also be categorized according to where the pain is felt. Heel pain, which is felt on the bottom of the heel, is the most prevalent form. On the other hand, some persons may feel pain in the foot’s ball or arch. The location of the inflammation in the plantar fascia will determine the kind of discomfort that is felt.
All things considered, plantar fasciitis is a common illness that is treatable with the right care and medication. People can collaborate with their medical specialists to create a treatment plan that is most suited to their unique needs by being aware of the many types of plantar fasciitis.
Causes and Symptoms of Plantar Fasciitis
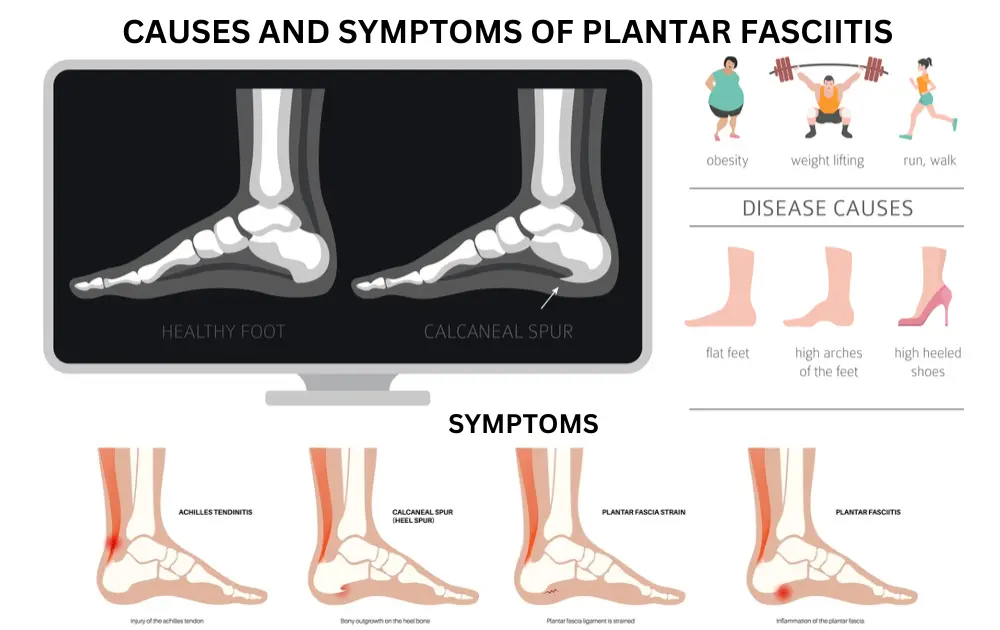
Causes
Pain in the heel and arch of the foot are symptoms of plantar fasciitis. The plantar fascia, a substantial strip of tissue that connects the heel bone to the toes, becomes inflamed, giving rise to it. The plantar fascia supports the arch of the foot and works as a shock absorber for the foot.
Stress on the plantar fascia is the most frequent cause of plantar fasciitis. There are numerous causes for this, including:
- Overuse: Repetitive strain on the plantar fascia can result in small rips in the tissue, which can cause pain and irritation.
- High arches or flat feet: Due to abnormal foot mechanics that place additional strain on the plantar fascia, people who have high arches or flat feet are more susceptible to developing plantar fasciitis.
- Tight calf muscles: Tight calf muscles can increase the stress placed on the plantar fascia and the Achilles tendon.
- Obesity: Being overweight increases the risk of developing plantar fasciitis and places additional strain on the plantar fascia.
- Poor footwear: The plantar fascia can experience additional stress from shoes that do not offer enough support or cushioning.
Other variables that can contribute to plantar fasciitis include:
- Age: People between 40 and 60 are more likely to develop plantar fasciitis.
- Certain types of exercise: Exercises that strain the heel and its connective tissue, such as long-distance running, ballet, and aerobic dance, might hasten the development of plantar fasciitis.
- Certain professions: People in factory jobs and instructors who must stand or walk for lengthy periods of time on hard surfaces are more likely to develop plantar fasciitis.
In order to prevent and treat plantar fasciitis, it is crucial to understand its causes. People can reduce their risk of getting plantar fasciitis and hasten the healing process by treating the underlying reasons for the ailment.
Signs or Symptoms
A common foot condition called plantar fasciitis is characterized by pain in the heel or arch of the foot. Usually, the pain is greatest in the morning or after spending a lot of time sitting or standing. The following are some typical signs of plantar fasciitis:
- Heel pain: The most typical sign of plantar fasciitis is heel pain. The bottom of the heel is typically where the pain is felt, and it can be either severe or dull. When you first get out of bed in the morning or after spending a lot of time sitting, it is frequently worse.
- Foot pain: Pain in the foot arch is another symptom of plantar fasciitis. This discomfort, which can be either intense or mild, tends to get worse after spending a lot of time standing or moving around.
- Stiffness: People who have plantar fasciitis may feel stiff in their ankles or feet. After a lengthy period of sitting or in the morning, this stiffness could be exacerbated.
- Oedema (Swelling): Around the heel, some persons with plantar fasciitis may suffer oedema. This oedema could be little or significant.
- Achilles tendon tightness: Plantar fasciitis may result in Achilles tendon tightness. It could be challenging to walk normally or flex your foot as a result.
To receive a precise diagnosis and treatment plan, you must speak with a medical specialist (orthopaedic specialist) if you are experiencing any of these symptoms.
Now, if we are talking about signs and symptoms so let’s find out in this link – If heel pain is a sign of cancer.
Diagnosis of Plantar Fasciitis

The medical history and physical examination of the patient are used to make the diagnosis of plantar fasciitis. The medical professional will look for sore spots on the foot while performing the examination. Finding the source of the pain can be aided by knowing where it is. An X-ray or an MRI may be prescribed in some situations to rule out other disorders that can cause heel pain even though imaging tests are typically not required.
Pain in the heel or arch of the foot is a common symptom of plantar fasciitis, especially when standing or walking after periods of rest. The discomfort is frequently reported as being acute, stabbing, or scorching. Additionally, particularly first thing in the morning, patients may feel stiffness or pain in the foot.
Age, obesity, high-impact sports like running or leaping, and wearing shoes with inadequate arch support are all risk factors for plantar fasciitis. Patients with high arches or flat feet may also be more vulnerable.
Additionally, a walking or motion analysis (gait analysis) may be performed by a medical professional to evaluate the patient’s gait and identify any deviations that could be contributing to the patient’s plantar fasciitis. This can possibly aid (help) in directing treatment suggestions and avoiding further injuries.
In general, quick diagnosis and treatment of plantar fasciitis can aid (help) in symptom relief and stop additional issues. Patients who have had heel discomfort for more than a week should consult a doctor to identify the cause and get the right care.
Stages of Plantar Fasciitis
A typical condition that causes discomfort in the heel and the bottom of the foot is plantar fasciitis. Furthermore, Plantar Feciitis can be divided into four stages:-
- Stage 1: Early Stage
- Stage 2: Mid-Stage
- Stage 3: Advanced Stage
- Stage 4: Chronic Stage
Stage 1: Early Stage
- People may feel some mild discomfort or pain in the heel or arch of the foot during this initial phase.
- Getting out of bed in the morning or standing up after sitting for a while are common examples of when pain is present after periods of inactivity.
- Sporadic symptoms are possible, and they usually get better with rest and stretching.
Stage 2: Mid-Stage
- At this point, the feeling of pain is more constant and can happen when running or walking.
- Additionally, pain may appear after extended durations of standing.
- In the plantar fascia, swelling and inflammation are frequently more noticeable.
Stage 3: Advanced Stage
- Pain worsens and persists in the advanced stage, frequently affecting daily activities and quality of life.
- Other parts of the foot could experience pain in addition to the heel.
- Additionally, there is a higher chance of getting side effects like heel spurs.
Stage 4: Chronic Stage
- The worst stage of plantar fasciitis is at this point.
- Pain is continuous and incapacitating because chronic inflammation and tissue damage are predominant.
- Significant functional and mobility limitations exist.
10 Common Methods for Treatments of Plantar Fasciitis
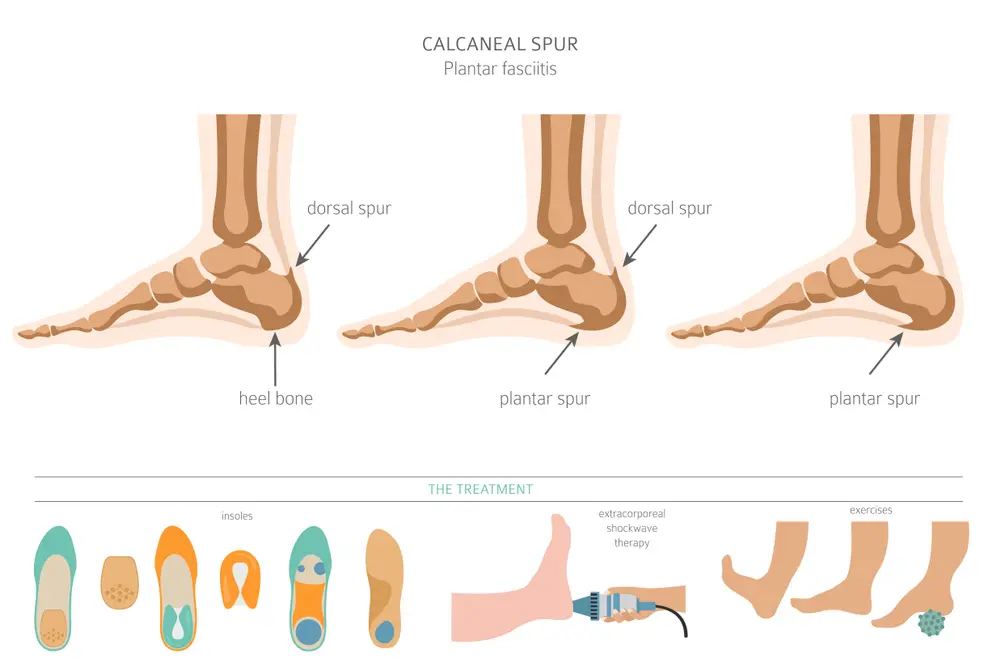
From natural remedies to medical intervention, there are several ways to treat plantar fasciitis. 10 common methods to treat plantar fasciitis are:
- Rest and Ice: Reducing swelling and relieving discomfort can be accomplished by resting the foot and administering ice to the injured region.
- Anti-inflammatory Medications: Drugs or medicines that are available over-the-counter to treat inflammation and discomfort include ibuprofen and naproxen.
- Physical Therapy: Physical therapy can assist in stretching and strengthening the muscles and ligaments in the foot and lower leg, which can help to reduce discomfort and fend off further injuries.
- Shoe Inserts: Inserts for shoes, such as orthotics or heel cups, can support and cushion the foot, easing pressure on the plantar fascia.
- Calf muscle stretches: Stretching your calf muscle can help relieve pain and ease strain on the plantar fascia.
- Arch Supports: Arch supports can help provide additional support to the foot and reduce stress on the plantar fascia.
- Night splints: While you sleep, night splints can help stretch the plantar fascia and Achilles tendon, which helps reduce morning stiffness and soreness.
- Plantar Fasciitis Socks: Plantar fasciitis Socks can aid (help) in compressing and supporting the foot, which helps reduce discomfort and swelling.
- Extracorporeal Shock Wave Therapy (ESWT): A medical procedure called extracorporeal shock wave therapy (ESWT) uses shock waves to boost healing in the injured area.
- Surgery: To remove injured tissue or heal the plantar fascia in extreme situations, surgery may be required.
It is significant to remember that the results of these treatments can change depending on the severity of the ailment and the patient’s response to treatment. It is advised to speak with a medical expert to decide the best course of action for your particular case of plantar fasciitis.
How to Cure Plantar Fasciitis in One Week? – One Week Treatment Plan

Although plantar fasciitis can be an uncomfortable and irritating condition, with the correct treatment strategy, the symptoms can be reduced in just one week. This section will provide a complete one-week plan worth of instructions, including rest, ice, stretching, strengthening, maintenance, and prevention. These Includes:-
- Day 1-3: Rest and Ice
- Day 4-5: Stretching and Strengthening
- Day 6-7: Maintenance and Prevention
Day 1-3: Rest and Ice
Resting the injured foot is the first step in treating plantar fasciitis. One should avoid foot-stressing exercises like running and hopping. Instead, they should strive to limit their time on their feet and avoid standing or walking for extended periods.
Ice can also aid (help) with pain relief and inflammation reduction in addition to rest. Several times a day, apply an ice pack to the affected area for 15-20 minutes at a time to assist ease pain and swelling.
Day 4-5: Stretching and Strengthening
It’s time to start stretching and strengthening the foot and ankle after a few days of rest and ice. This can aid (help) in increasing flexibility and lower the chance of suffering another injury.
Some effective stretches for plantar fasciitis include:
- Calf stretch: Stretch your calves by placing one foot in front of the other while facing a wall. Keep the front leg bowed and the back leg straight. When you feel a stretch in the back leg’s calf muscle, lean forward.
- Toe stretch: Lie on the ground with one foot and cross the other foot over the knee. When you feel a stretch in the sole of the foot, use your palm to gently bring the toes back toward the ankle.
- Towel stretch: A towel should be wrapped around the ball of one foot as you sit with your legs straight in front of you. When you feel a stretch in the calf muscle, gently draw the foot toward you while using the towel.
For people with plantar fasciitis, strengthening activities can be beneficial. Good choices comprise:
- Toe curls: Place a towel or other small object under your toes while sitting with your feet flat on the ground. Take hold of the towel or other item with your toes and hold on for a few seconds before letting go.
- Heel raises: Standing with your feet shoulder-width apart, elevate your heels slowly onto your toes. Hold for a few seconds for a while before lowering back down.
Day 6-7: Maintenance and Prevention
The focus of the treatment plan for the last few days should be on maintenance and prevention. This entails (involves) maintaining the foot and ankle’s flexibility and strength as well as taking precautions to avoid further harm.
Here are some pointers for keeping your feet healthy:
- wearing sturdy footwear with adequate arch support.
- Avoiding shoes with little to no support and high heels.
- using orthotic inserts to add additional support and cushioning.
- Upkeep a healthy weight to relieve foot pressure.
People with plantar fasciitis can significantly reduce their pain and improve their overall foot health by adhering to this one-week treatment plan.
My Personal Experience
“Hello, I’m Sunil, and the article I’m sharing with you today is deeply personal to me because it revolves around a condition I once battled fiercely – Plantar Fasciitis.
A few months ago, on a seemingly ordinary day, I was on my way home from work when an innocent misstep on a wet stair led to a sudden twist of my right foot. At first, the pain seemed manageable, so I continued on my way. However, by the time I reached home, my foot had swelled up, and the pain had escalated to an unbearable level. Every step became an ordeal, and I was in dire need of a solution.
Instead of rushing to the doctor’s office, I decided to take matters into my own hands. I delved into extensive online research about Plantar Fasciitis, watched countless videos, and gathered information about the most effective ways to treat this condition from the comfort of my home within just a week.
My journey towards curing Plantar Fasciitis in a week commenced with a crucial step – rest. For the initial two days, I allowed my foot to heal while applying ice (2 to 3 times a day), coupled with the use of pain relief spray and bandages. Although there was some improvement, the pain lingered, especially when walking on hard surfaces, so I avoided going barefoot.
Realizing that the road to recovery required more, I moved on to the next phase on the third day. I incorporated stretching and strengthening exercises like calf stretches and toe stretches into my daily routine. Even as I continued using pain relief spray and bandages, the pain subsided significantly, and by the end of the week, I was walking normally once again.
In just seven days, my condition had improved dramatically. I not only walked without pain but also reclaimed the joy of running. I am profoundly thankful that my journey led me to overcome Plantar Fasciitis within such a short span. While I understand that everyone’s experience may differ, I firmly believe that with the right treatment, most individuals can recover from Plantar Fasciitis in a matter of weeks or months.
Alternative Treatments
Alternative therapies can help with plantar fasciitis symptoms in addition to conventional medical approaches. Some of these remedies consist of:
- Acupuncture
- Chiropractic Care
- Massage Therapy
- Yoga and Stretching
Acupuncture
Thin needles are inserted into precise body locations during acupuncture. This is said to be an ancient Chinese medical procedure. It is believed that it aids (helps) in reducing inflammation and pain. Acupuncture treatments have been effective for some persons with plantar fasciitis.
Chiropractic Care
To treat pain and increase mobility, chiropractors manipulate the spine and other joints. Other methods, such as ultrasonography, may also be used by some chiropractors to aid (help) treat plantar fasciitis symptoms.
Massage Therapy
Blood flow can be improved and stress in the foot’s muscles and tissues can be reduced using massage therapy. This may ease (help) discomfort and increase mobility. To aid (help) in reducing inflammation and promoting healing, certain massage therapists may also apply essential oils or other topical remedies.
Yoga and Stretching
Stretching and yoga can ease tension in the foot’s muscles and tissues and increase flexibility. This may reduce the effects of plantar fasciitis. Yoga poses including the downward-facing dog, standing forward bend, and seated forward bend may be helpful for patients with plantar fasciitis.
The use of alternative therapies should not take the place of medical care, even though they may be beneficial for certain persons with plantar fasciitis. It is usually advisable to get medical advice before attempting unfamiliar medicines or treatments.
Short-Term Vs Long-Term Relief
Here is a table that contrasts the difference between short-term and long-term relief and the methods that can be used for treating plantar fasciitis over the long term and the short term:
| Aspect | Short-Term Relief | Long-Term Relief |
|---|---|---|
| Treatment Focus | Alleviating immediate pain and discomfort | Addressing the root causes and preventing recurrence |
| Methods | Rest, ice, compression, elevation (RICE), over-the-counter pain relievers, temporary arch supports, and cushioned footwear | Stretching exercises, physical therapy, custom orthotics, lifestyle changes, and strengthening exercises |
| Effectiveness | Provides temporary relief from pain and inflammation | Offers lasting relief by targeting underlying issues such as muscle imbalances and foot mechanics |
| Time Frame | Typically provides relief within days to weeks | May take several months to see significant improvement |
| Usage Duration | Used for a short period during acute pain episodes | Continued for an extended period to maintain foot health |
| Cost | Relatively low cost for short-term solutions | May involve higher costs for custom orthotics, therapy, or professional guidance |
| Risk of Dependency | Limited risk of dependency on short-term methods | Lower risk of dependency on long-term strategies, but consistency is key |
| Preventative Measures | Often does not address the root causes, making recurrence likely | Focuses on identifying and correcting the underlying factors to reduce the risk of recurrence |
| Professional Involvement | Minimal need for medical professionals in the short term | This may involve higher costs for custom orthotics, therapy, or professional guidance |
| Surgery | Rarely necessary for short-term relief | Considered in severe cases that do not respond to conservative measures |
Please be aware that each person’s level of success may differ with respect to these procedures, and that the most effective way to treat plantar fasciitis may be to combine both short-term and long-term relief techniques. For individualized guidance and treatment options, it’s crucial to speak with a healthcare expert.
Preventive Measures and Lifestyle Changes
Plantar fasciitis can be effectively managed and prevented with the use of preventative measures and lifestyle modifications. Here are some practical steps that might ease discomfort and encourage recovery:
- Weight Management
- Activity Modification
- Proper Foot Care
- Use of Supportive Devices
- Importance of Rest
Weight Management
It’s crucial to keep a healthy weight to relieve stress on the foot and avoid plantar fasciitis. Unneeded pressure from extra weight can cause the feet to swell and hurt. To relieve the pressure on their feet, those who are overweight or obese should aim to lose weight gradually.
Activity Modification
To lower their chance of getting the ailment, people who are prone to plantar fasciitis should change their physical habits. Running and jogging are examples of activities that should be cut back on or completely avoided. To reduce the stress on their feet, people can engage in low-impact activities like cycling or swimming.
Proper Foot Care
For those with plantar fasciitis, good foot care is essential. Shoes that are comfortable to wear and offer sufficient support can aid (help) in pain relief and rehabilitation. Additionally, people should refrain from going barefoot, particularly on hard surfaces, as this might make their condition worse. Regular massages to the affected area can also relieve pain and hasten recovery.
Use of Supportive Devices
In order to support the arch and ease pain, supporting devices like shoe inserts or orthotics can be used. These tools aid in assisting the even distribution of pressure across the foot and can reduce the likelihood of developing plantar fasciitis. The ideal kind of gadget for a person’s unique needs should be determined after consultation with a physician or podiatrist.
Importance of Rest
People with plantar fasciitis must get plenty of rest. Reducing physical activity and allowing the injured area to recover can help with pain management and healing. Depending on how severe the illness is, people should try to relax for at least a day or two. They should avoid standing for extended amounts of time and engage in low-impact exercises like yoga or stretching during this time.
People need to change their lifestyles and take preventive steps so that there are zero chances or fewer chances of getting plantar fasciitis and even speed up the healing process for those who are struggling with plantar fasciitis. Although these exercises might not offer a quick answer, it is crucial to remember that they might progressively aid in easing discomfort and enhancing general foot health.
Nutrition for Plantar Fasciitis

Even while there isn’t a specific diet that helps treat plantar fasciitis, adopting a balanced, healthy diet can assist in minimizing inflammation and speed up healing. Include the following essential nutrients in your diet:
- Omega-3 Fatty Acids
- Vitamin C
- Vitamin D
- Magnesium
- Anti-Inflammatory Foods
Omega-3 Fatty Acids
Omega-3 fatty acids are renowned for their ability to reduce inflammation. Fatty fish like salmon, sardines, and mackerel as well as flaxseeds, chia seeds, and walnuts are among the foods high in omega-3s. If you don’t consume enough omega-3-rich meals, you might want to think about taking a fish oil supplement.
Vitamin C
Antioxidant vitamin C helps lessen inflammation and encourage tissue healing. Citrus fruits, strawberries, kiwis, bell peppers, and broccoli are a few examples of foods strong in vitamin C.
Vitamin D
In addition to contributing to bone health, vitamin D may also lessen inflammation. Fatty fish, egg yolks, and fortified foods like milk and cereal are good sources of vitamin D. Consider getting some sun exposure or taking a supplement if you find it challenging to get enough vitamin D from meals alone.
Magnesium
A kind of mineral, Magnesium, can help in easing tension in the body and reduce swelling. Some of the excellent sources of magnesium are Nuts, seeds, whole grains, and leafy green vegetables.
Anti-Inflammatory Foods
Including anti-inflammatory foods in your diet, in addition to particular nutrients, can help lessen inflammation throughout the body. These consist of:
- Berries like strawberries, raspberries, and blueberries.
- Dark leafy greens like kale and spinach
- Spice with potent anti-inflammatory effects like turmeric
- Another seasoning with anti-inflammatory properties is ginger.
- Green tea, which has anti-inflammatory and antioxidant properties
Eating a balanced diet helps support the healing process and reduce inflammation, even though nutrition may not be enough to treat plantar fasciitis on its own.
Potential Risks and Complications
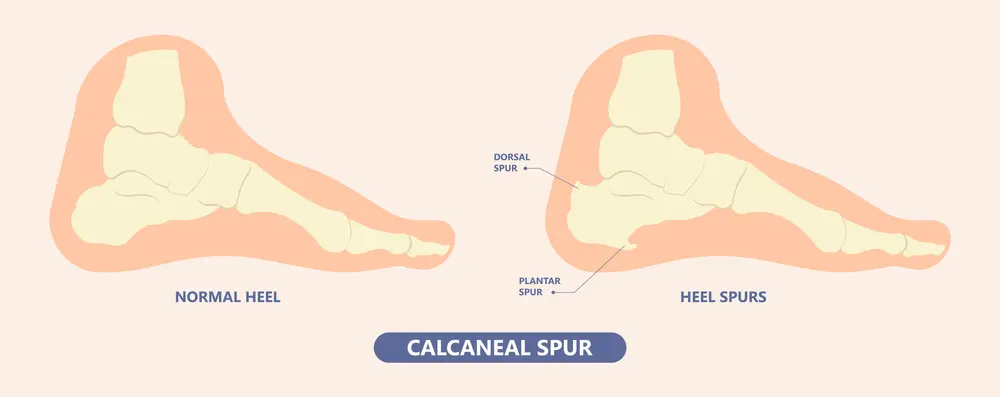
A prevalent condition that affects millions of individuals worldwide is plantar fasciitis. Although there are many efficient treatments available, it’s crucial to be informed of any hazards or difficulties this ailment can bring with it.
Heel spur formation is among the most frequent dangers connected to plantar fasciitis. On the base of the heel bone, there may form bony growths known as heel spurs. They frequently result in chronic inflammation of the plantar fascia and can be quite painful and uncomfortable.
The emergence of chronic discomfort is yet another potential side effect of plantar fasciitis. Plantar fasciitis can develop into a chronic condition that makes it difficult to walk or exercise if it is not treated. This may necessitate more harsh treatment alternatives and result in a decline in general quality of life.
Rarely, plantar fasciitis can cause stress fractures, tendinitis, or nerve damage in the feet and ankles. These issues can be very significant and may need to be fixed surgically.
If you believe you might get plantar fasciitis, you must immediately visit a doctor. You can avoid these potential risks and concerns and return to normal activities more quickly by receiving early detection and treatment.
Plantar Fasciitis Case Study
A common foot condition called plantar fasciitis can cause pain and discomfort in the foot’s heel and arch. Let’s look at a patient with plantar fasciitis and how they were able to find relief in a case study.
Patient Background
The patient, a female 45-year-old, has been dealing with heel pain for a while. She claimed that the discomfort was worse in the morning when she first awoke and progressively got better throughout the day. However, after prolonged standing or walking, the pain would return.
The patient had swelling and pain in the heel area, according to the examination. To rule out any fractures or other structural issues, X-rays were obtained.
Treatment Plan
The patient was instructed to take it easy and stay away from any painful activities. She was told to do plantar fascia and calf muscle stretches, as well as freeze the problematic area many times a day for 15-20 minutes at a time.
The patient also received a set of personalized orthotics to support her foot arch and ease pressure on her plantar fascia. To help her manage the pain and inflammation, nonsteroidal anti-inflammatory medications (NSAIDs) were also provided.
Results
The patient indicated that his or her discomfort and oedema had significantly decreased after following the treatment plan for one week. She was able to stand and stroll for extended stretches of time without getting tired.
The patient continued her stretching routine and wore her personalized orthotics for several weeks. She also had physical therapy to bolster the muscles in her foot and ankle and increase her range of motion.
The patient’s plantar fasciitis had totally resolved by the end of the six-week therapy term, and she was able to resume her regular activities pain-free.
Conclusion
Plantar fasciitis is a painful and frustrating condition that can be resolved in a week or less With proper care. Patients can reduce their swelling, pain, and other symptoms while also promoting the repair of the plantar fascia by combining rest, ice, stretching, and other treatments.
Physical therapy is one of the best remedies for plantar fasciitis. Physical therapists can demonstrate to patients stretching and strengthening techniques for the Achilles tendon and plantar fascia. Additionally, they can instruct patients on how to utilize night splints to keep the plantar fascia stretched while they sleep and athletic taping to support the bottom of their feet.
Patients may also benefit from at-home treatments like stretching, massaging, and icing the affected area in addition to physical therapy. In order to lessen pain and inflammation, they can also use over-the-counter painkillers like nonsteroidal anti-inflammatory medicines (NSAIDs).
Patients who have persistent or severe plantar fasciitis could need more aggressive therapies including shockwave therapy or corticosteroid injections. These procedures should only be carried out with a doctor’s supervision, though.
Overall, treating plantar fasciitis in one week involves a multimodal strategy that takes care of the condition’s underlying causes and encourages the plantar fascia to repair. Patients can quickly return to their regular activities and have less pain and inflammation with the proper treatment strategy.
People Also Ask (FAQs)
Q: What are some effective exercises for plantar fasciitis relief?
A: Exercises that stretch the muscles can aid in reducing plantar fasciitis pain. Calf stretches, toe stretches, and towel stretches are a few good workouts. Stretching the plantar fascia and Achilles tendon using these activities will help lessen discomfort and inflammation.
Q: What are some recommended anti-inflammatory creams for plantar fasciitis?
A: For people with plantar fasciitis, ibuprofen gel, diclofenac gel, and piroxicam gel are among the suggested anti-inflammatory creams. These lotions might aid in easing discomfort and swelling in the affected area.
Q: Can plantar fasciitis be cured in one week? If so, how?
A: Although plantar fasciitis can be a persistent illness, the symptoms can usually be reduced within a week. Rest, ice, stretching, and wearing supportive shoes are a few strategies for doing this. It is important to see a doctor If the pain doesn’t go away.
Q: What are some quick and effective ways to heal plantar fasciitis?
A: Rest, ice, and stretching are some simple and efficient treatments for plantar fasciitis. Additionally, it’s crucial to wear supportive shoes and stay away from aggravating activities.
Q: Is soaking feet in warm water helpful for plantar fasciitis?
A: Plantar fasciitis discomfort can be reduced by soaking feet in warm water. Epsom salt can be added to the water to further aid in relieving inflammation.
Q: What are some things to avoid doing when suffering from plantar fasciitis?
A: Avoiding foot-stressing activities like running or leaping is crucial while dealing with plantar fasciitis. Additionally, it’s crucial to stay away from footwear with inadequate arch support.
Q: What is the fastest way to cure plantar fasciitis?
A: Although there isn’t a single effective treatment for plantar fasciitis, there are a number of techniques to reduce the symptoms. Rest, ice, stretching, and wearing supportive shoes are a few strategies for doing this.
Q: What deficiency causes plantar fasciitis?
A: Although the precise cause of plantar fasciitis is unknown, some studies suggest that a lack of vitamin D may be a contributing factor.
Q: Can lack of vitamin D cause plantar fasciitis?
A: According to certain research, plantar fasciitis may be exacerbated by a vitamin D deficiency. However, More study is necessary to support this.
Q: What foods cause plantar fasciitis?
A: No evidence exists to support the claim that any particular foods promote plantar fasciitis.
Q: Is plantar fasciitis caused by uric acid?
A: Uric acid does not induce plantar fasciitis. The band of tissue that connects the heel bone to the toes, the plantar fascia, becomes inflamed, which is the source of the condition.
Q: What nutritional deficiency causes plantar fasciitis?
A: The exact origin of plantar fasciitis is unknown, but some research indicates that vitamin D deficiency may be a contributing factor.
Q: What foods help plantar fasciitis?
A: There is no proof that any particular foods can help with plantar fasciitis symptoms.
Q: Are eggs good for plantar fasciitis?
A: There is no proof that eggs have a particular impact on plantar fasciitis. Instead of focusing on certain foods, managing plantar fasciitis entails treating variables like inflammation and poor foot mechanics. Concentrate on eating a generally healthy diet and seek out specific guidance from a healthcare professional.












